Robustness of Transformer-Based Fluence Map Prediction Under Clinically Realistic Perturbations
arXiv cs.CV / 5/5/2026
📰 NewsIdeas & Deep AnalysisModels & Research
Key Points
- The study evaluates how a two-stage transformer pipeline for IMRT fluence map prediction holds up under clinically realistic distribution shifts and perturbations.
- It compares different transformer attention designs (fluence-stage transformer backbones including hierarchical, global, and hybrid attention) trained with a physics-informed loss that enforces energy consistency.
- Robustness degrades smoothly under moderate geometric/radiometric changes, but the model can experience sharp failures under severe rotations and strong noise.
- Hierarchical transformers such as SwinUNETR show more favorable behavior, with slower increases in upper-quartile energy error under perturbations.
- The authors find that relying on SSIM alone is insufficient for clinically meaningful error assessment, motivating physics-informed evaluation metrics beyond image similarity.
Related Articles
Ten Reddit Threads That Made AI Agents Look More Like Infrastructure Than Hype
Dev.to
From Demos to Guardrails: 10 Reddit Threads Tracking the AI-Agent Shift
Dev.to
Ten Reddit Posts That Split the AI-Agent Conversation Into Four Live Debates
Dev.to
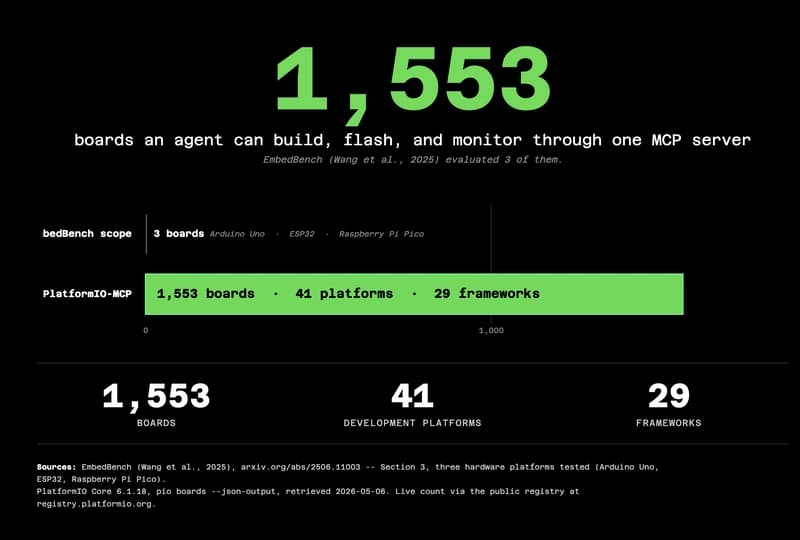
The 55.6% problem: why frontier LLMs fail at embedded code
Dev.to

Four CVEs in a week, all the same shape: when agents execute LLM-generated code
Dev.to